Staff ingenuity and determination is keeping elective care going
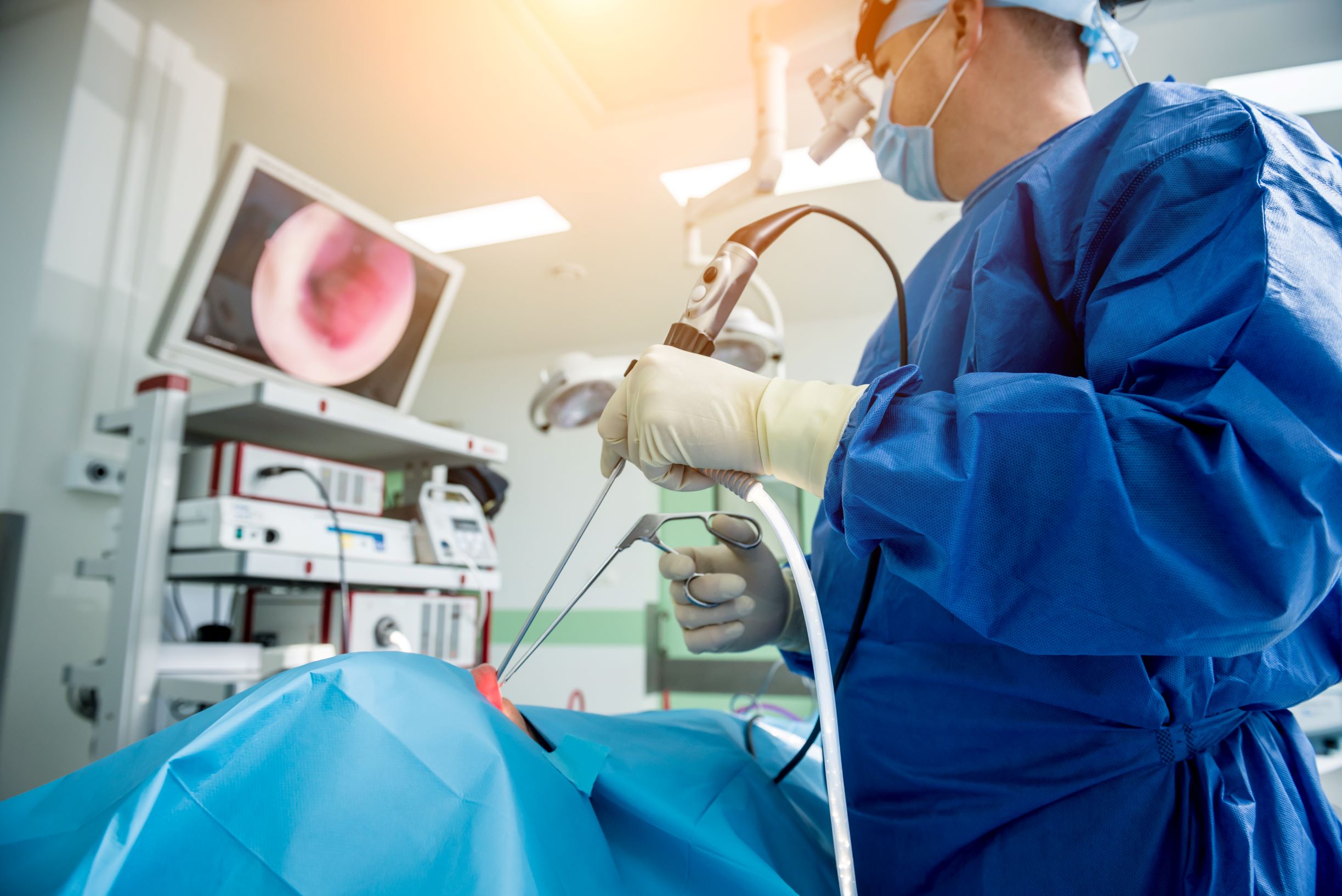
During a testing period for healthcare, Lindsay Dransfield, Commercial Director for Vanguard Healthcare, pays tribute to health and care staff across the country. In particular, she highlights the innovative ways in which staff are optimising the healthcare estate to maintain service delivery.
The current strain on health and care services is unimaginable and the growing backlog in elective care is ominous, but in the face of unprecedented adversity, the NHS is achieving remarkable things. We can see this tireless work reflected in the most recent figures on diagnostic activity and waiting times in England, released last week.
There were real signs of recovery in endoscopy activity last autumn – despite the rise in Covid-19 cases. While activity remains below last year, it had reached 86 per cent of last November’s level and was broadly in line with December 2019. What’s more, the number of patients seen within the 6-week target has increased markedly month-on-month and the total waiting list for endoscopy actually contracted in both October and November.
Although elective care backlogs remain at historic highs, waiting times for patients would have been even longer without the efforts of hospitals and trusts taking decisive action to keep essential care going. By very quickly adapting the use of both internal and external space in order to minimise any disruption to non-urgent care during the pandemic, they have helped prevent an even bigger crisis.
In particular, the dedication and the extraordinary resilience of clinical staff that are working in difficult conditions throughout the pandemic to deliver vital patient care warrants more than a passing mention. From a Vanguard perspective, all of our clinical staff have had to adapt to new conditions, while some have taken on completely different roles during Covid-19, or joined host hospitals’ teams to provide support elsewhere on the site.
We are honoured to have worked with a number of trusts who have taken positive action to ensure the continuation of elective surgery and diagnostic procedures as far as possible.
A flexible resource
An example of how flexible healthcare facilities can be adapted as circumstances change is provided at our bespoke ophthalmic hub situated at Royal Preston Hospital. Initially installed to add capacity for cataract surgery, the use of the unit was flexed during Covid-19.
The hub, which incorporated two Vanguard laminar flow theatres, was in daily use before Covid-19 struck, helping to reduce waiting lists for conditions such as glaucoma, ocular plastics, cancers of the eye and cataracts. In one of the theatres, the team had carried out more than 100 cataract procedures in just two weeks.
When elective surgery was cancelled back in April, the hospital realised that the hub was ideal for use for emergency surgeries and smaller plastic surgeries. It also aided overall patient flow, as patients could be assessed and admitted directly onto the hub, via a separate pathway to the main hospital admission area.
Dr Shveta Bansal, Consultant Ophthalmologist at Lancashire Teaching Hospitals NHS Foundation Trust and Clinical Lead for the project, said at the time: “Having the Vanguard unit as a standalone facility separate from the hospital was a huge asset during the early stages of Covid-19.”
Continuing elective care
At the Shrewsbury and Telford Hospital NHS Trust, a mobile operating theatre and ward had been set up at the Princess Royal Hospital in Telford in 2019, supported by a team of four Vanguard staff members. Specialist oral surgery, ENT and urology patients accounted for the majority of the work on the unit, which was focused on procedures with long waiting lists, and prior to the pandemic, the unit saw between 8 and 10 patients a day on average.
Since the start of Covid-19, the unit has been successfully operating as a ‘cold’ site for the Trust, allowing key procedures to continue. The unit is completely separate from the main hospital and the staff are a designated team, not working elsewhere within the hospital.
Neil Rogers, Assistant Chief Operating Officer for Scheduled Care at The Shrewsbury and Telford Hospital NHS Trust, said: “Having the unit separate to the hospital is key for patient safety and the patients have been very happy to attend because of that separation and the ring-fenced group of staff.
“The team have been really helpful, they are really part of our collective team and it has been great to have that additional resource and expertise on site. Even when the unit was on downtime, we knew we could turn to them if they were needed.”
Improving patient flow
Another hospital that quickly adapted to the new circumstances was the Royal Infirmary of Edinburgh. In 2019, a temporary minor injuries unit, using a combination of a mobile laminar flow operating theatre and a number of modular buildings, was set up at the site to improve patient flow in the A&E department.
But with fewer people presenting to A&E during the pandemic, fewer people were also being directed to the MIU, while at the same time, additional space was urgently needed in other parts of the hospital. The facility was adapted to RIE’s changing infrastructure requirements within a very short timescale.
Being accessible from the existing A&E department, and having its own reception and waiting area, the MIU facility has proved versatile. It has been repurposed twice during the course of the pandemic, first as a surgical admissions ward, and later, for use as an emergency department observation area, also bringing a change of role for Vanguard’s staff on the unit.
It is now used to help keep beds in the emergency department next door for patients needing more urgent care, while those not in need of one-to-one nursing can be supported in the former MIU.
Reassuring patients
Modular and mobile wards are not only being used to supply additional hospital bed spaces, but also to provide additional reassurance for patients. This was the case at Kettering General Hospital in the UK, which commissioned a modular ward at the start of the pandemic to provide a Covid-free zone.
A bed modelling exercise at the start of the pandemic suggested the hospital may need additional bed capacity to deal with the crisis effectively, and the Trust decided to commission a modular ward to create another ‘green’ zone, away from Covid-19 areas, where at-risk patients could be safely cared for.
As well as providing the hospital with temporary additional bed capacity for non-Covid patients, its position on site offers reassurance for those who may be worried about attending hospital during the pandemic. The plan has allowed the Trust to retain additional Covid-19 capacity within the hospital for the second wave, which was the intention at the start.
The modules were built off-site by Young Medical, Vanguard’s specialist modular ubsidiary, and the stand-alone ward facility was completed within a period of just five weeks, despite the restrictions imposed by the lockdown protocol that was in place at the time.
Dedication and commitment
Covid-19 has brought extensive challenges to our colleagues right across the NHS, and Vanguard is honoured to have been able to contribute to their efforts to deliver essential patient care in any way possible. NHS staff have shown exceptional resilience as they have adapted to new conditions and continued to put patients first.
That goes for Vanguard’s own teams too. Many of our staff members have suddenly found themselves working in a different facility, at a different hospital or location, with different working hours, learned new skill sets, and in many cases have been given new responsibilities or have moved from elective to emergency care.
Some of our team members work away for long periods of time, and in addition to work-related changes, they have also faced additional challenges, such as their hotels closing down and not being able to see their families during breaks due to the risk of spreading the virus. They have made huge sacrifices in order to keep supporting hospitals.
Vanguard’s non-clinical staff have also overcome many additional challenges during the pandemic. Setting up a new healthcare facility requires site surveys, testing and assessments to be undertaken, units or modules to be refitted and transported, and in some cases construction or enabling works to be completed – all of which has been much more challenging due to restrictions during the pandemic.
Their efforts, and those of our colleagues across the NHS are making a huge difference to individual patients’ lives, and are keeping rising lists at bay as far as possible, even if the results are not always obvious when looking at performance data.
