Trials begin for smart wound sensors that could reduce diabetes-related amputations

Landmark study aiming to deliver a step change in the care of chronic wounds and reduce healthcare costs for wound management has begun patient trials in people with diabetes-related foot ulcers.
The study, being conducted at University Hospitals of Derby and Burton NHS Foundation Trust, will see ten patients with diabetes-related foot ulcers have dressings applied and monitored on a fortnightly basis for a total of eight weeks per patient. During appointments, the wounds will be assessed, and smart dressing applied for up to one hour under observation while measurements are taken.
Researchers at the University of Nottingham have received a £902,524 grant from the Medical Research Council to develop a smart wound dressing embedded with optical fibre sensors to assess whether affected tissue is healing or infected.
Wound management costs stand at £8.3 billion a year, more than four per cent of the NHS budget, with diabetes-related foot ulcers representing between £837 and £962 million of the cost. These hard-to-heal wounds are at the centre of the project, as better monitoring has the potential to reduce the more than 7,000 lower limb amputations carried out for people with diabetes in England every year.
Professor Steve Morgan, Co-Director of the Centre for Healthcare Technologies and Professor of Biomedical Engineering at the university, said: “Currently, regular wound redressing is the only way to visually assess healing rates, which can be detrimental as it can encourage infection and disrupt progress – not to mention the resulting economic burden on NHS resources.
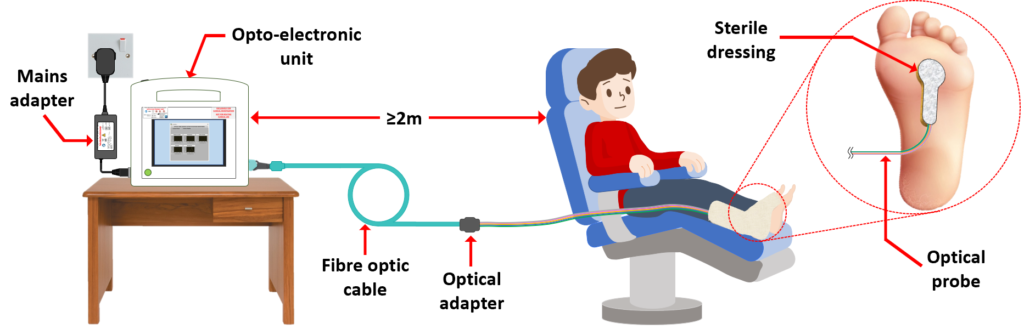
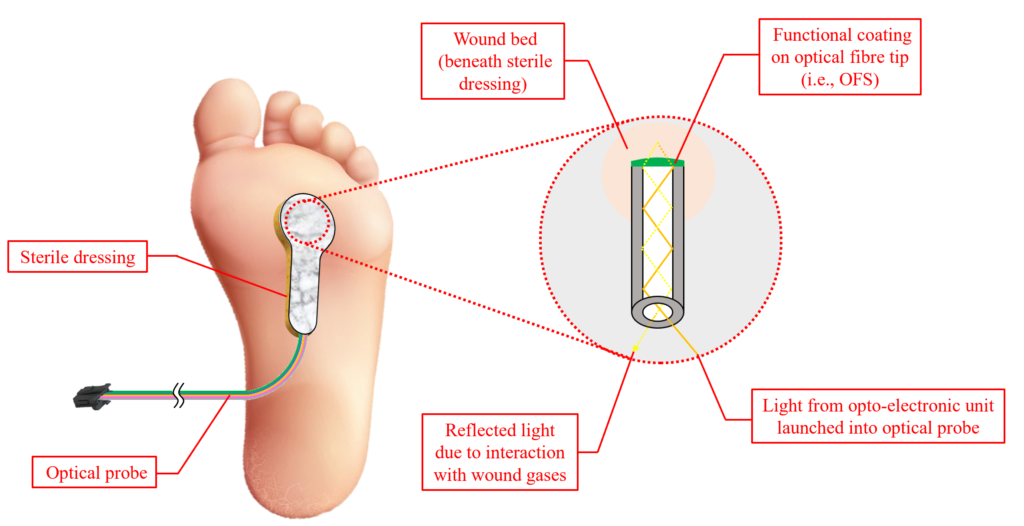
“Our smart wound dressing addresses this through the incorporation of optical fibre sensors, which can remotely monitor multiple factors associated with wound management, such as temperature, humidity and gases associated with healing and infection. This has the potential to indicate the optimum time for changing the dressing and could alert clinicians about whether an intervention is required for an infected or slow-healing wound. If successful, the impact would be a reduction in the number of healthcare appointments along with improved patient care.”
Professor Fran Game, Consultant Diabetologist and Clinical Director of Research and Development and the Derby Clinical Trials Support Unit at University Hospitals of Derby and Burton NHS Foundation Trust (UHDB), said: “Technologies to monitor wounds remotely and assess when things are going well or not so well, have the potential to have a significant impact on patients’ lives and health service costs. If we knew that a wound was healing well without having to use healthcare professionals time just to visually inspect it, it would make a huge difference to the NHS.
“Equally, knowing very quickly that wound healing had stalled, or an infection had developed, would mean that we could commence appropriate treatments much more promptly which would improve outcomes.
“I’m thrilled that the first trials of this device are being conducted at UHDB and that patients with diabetes will have the opportunity to support such ground-breaking research.”
Although the dressings will cost more than an average dressing up front, researchers hope to prove that this will be offset by fewer dressing changes or clinical visits and a reduced healing time.
Dr David Gomez, Assistant Professor in Optical Fibre Sensing for Healthcare and Medical Devices from the Faculty of Engineering, University of Nottingham, said: “Even a ten per cent reduction in costs associated with visits and appointments would provide significant annual savings of approximately £300 million for the NHS, but this is just one of the elements we’re looking to achieve through this research.
“If we’re able to generate a better understanding of ulcer healing and monitoring, we should be able to drastically reduce the number of amputations for future patients, because intervention when a wound gets infected will be quicker and more accurate, and usher in a new approach to chronic wound care.”
The project team includes clinicians at University Hospitals of Derby and Burton NHS Foundation Trust, Nottingham-based smart textiles company Footfalls and Heartbeats, and the Clinical Engineering Department at Nottingham University Hospitals NHS Trust.
