Technology is often a hard sell, but it has never been more valuable

George Batchelor, Co-Founder and Director of Edge Health, considers the effects of advances in technology will have upon health service delivery.
It is a full year since Covid-19 was first documented. The impact across society and the NHS has been vast and profound. Globally there have been nearly 1.8 million deaths – over 75,000 of these have been in the UK, hundreds have been clinicians.
Over the period, the NHS has also seen a colossal increase in waiting times. Over 140,000 people have now been waiting over a year for their treatment.
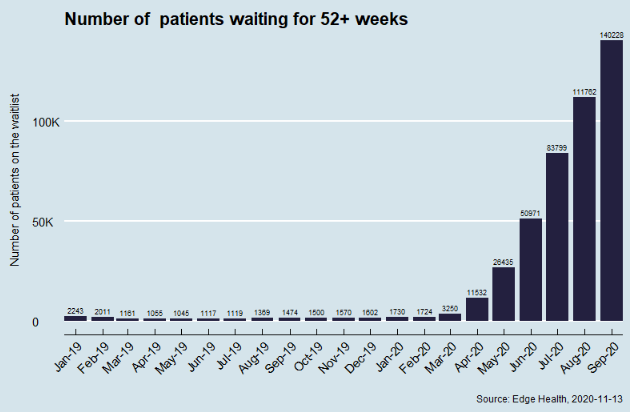
Compared with 2019, there are also a massive number of people who have not been referred for treatment – over five million. It is unclear exactly what has happened, but these do appear to be slowly returning. This increase in demand over the next few months coupled with reduced capacity due to introduced cleaning and safety measures since March 2020 could lead to the NHS waiting list growing to over 10 million by April 2021.
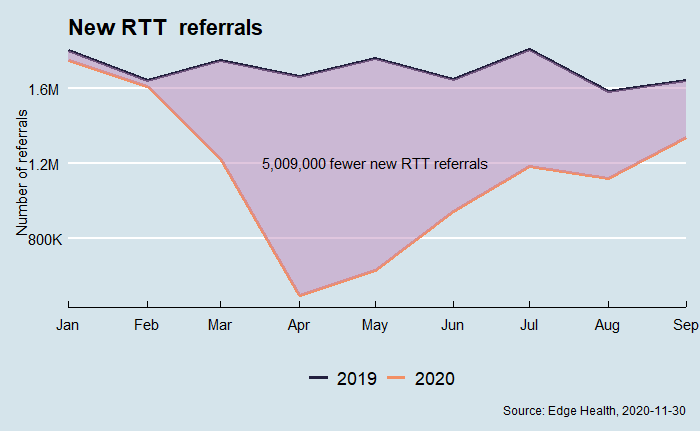
In our work with RM Partners, we have seen how different parts of the system are using data to build a coherent understanding of potential demand and system capacity. This has allowed essential services to be maintained at a system level – even during the crisis.
It is clear that the outlook for the NHS is exceptionally challenging, with demand outstripping capacity in many areas. This could have been far worse had it not been for the monumental efforts to scale up the use of video technology across the NHS earlier this year.
The programme, which started as a small pilot in NHS Improvement in 2019, became a national roll-out in March and has become one of the most successful technology adoptions in history. Within a few weeks, the NHS was routinely delivering video consultations – there have now been over 1.4 million.
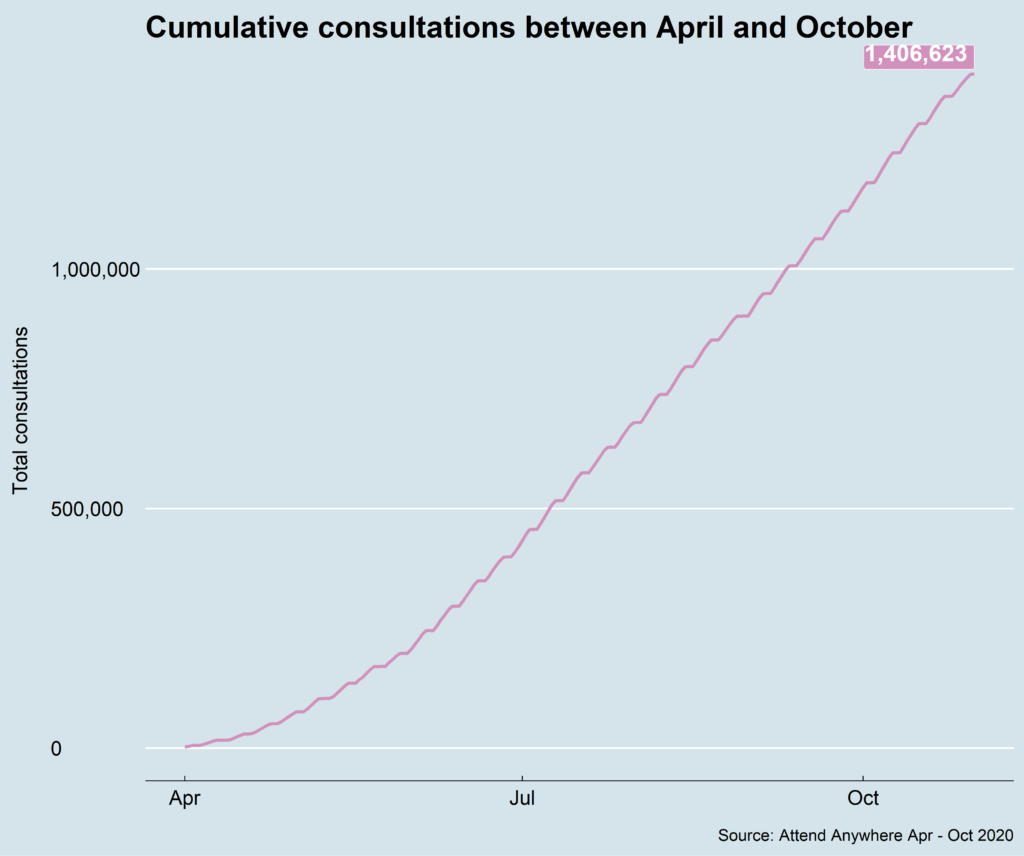
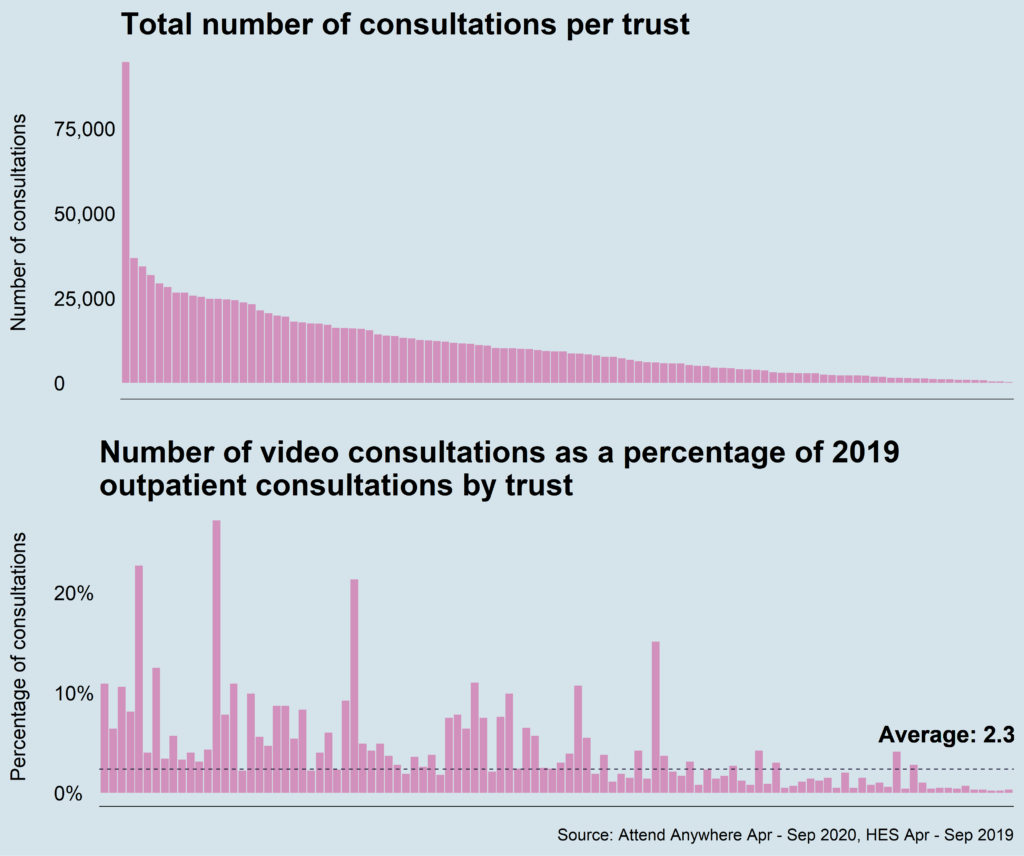
At some trusts, over 10 per cent of their 2019 outpatient activity levels are being delivered by video. This is a huge achievement and surpassed any target that would have been considered reasonable a year ago.
Covid-19 forced this rapid shift to video technology, but the gains are much broader than just keeping people out of hospitals.
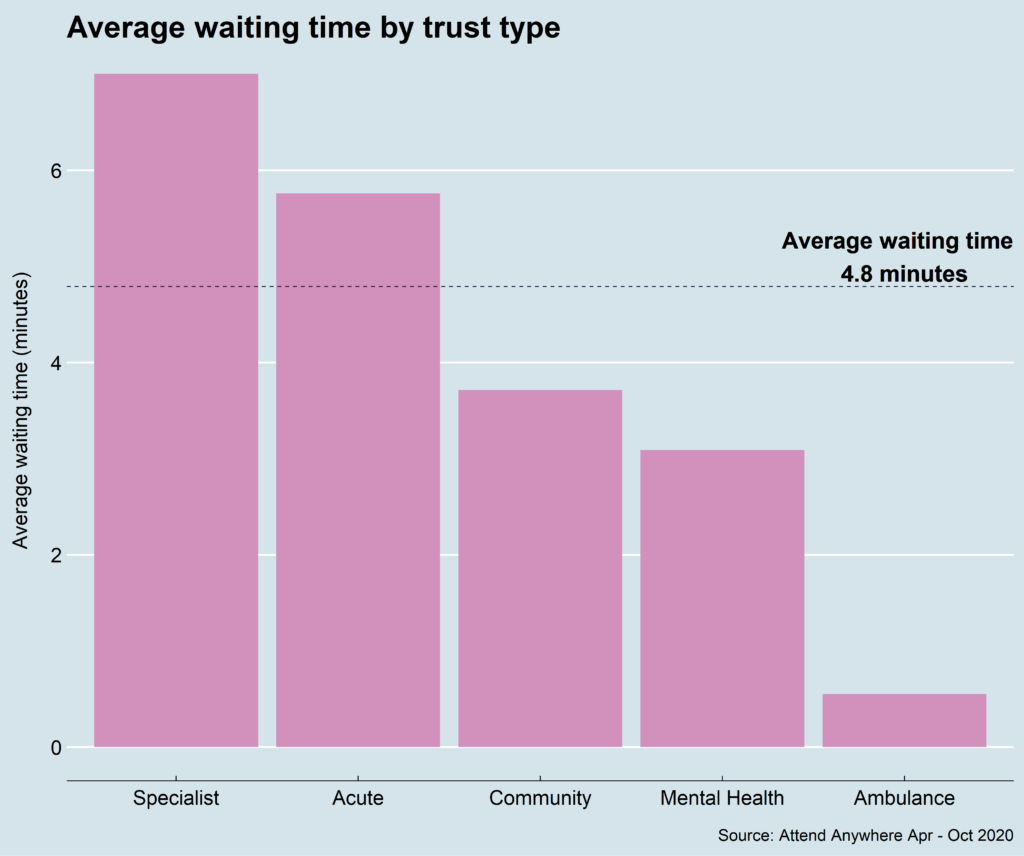
Video has also allowed flexible working for staff. The technology is more convenient for patients: average travel has been cut from a 20-mile round trip via a busy hospital car park, to a short walk to the sofa via the kettle. The shift to video has also reduced the average waiting time from over an hour in a hospital waiting room to less than five minutes. Like many other technologies, these benefits existed pre-pandemic and simply needed a catalyst to drive their uptake.
Addressing the backlog
Now, with the NHS waiting list approaching 10 million, it is critical to use data and technology to help.
Improved prioritisation and scheduling of waiting lists offers enormous potential to hospitals that want to maximise the use of their capacity. For example, our work with South Tees saw the development of Space Finder – a tool that uses artificial intelligence to optimise theatre scheduling. This unlocked enough capacity to push non-core activity back into core hours, improving safety and reducing the cost of overtime.
Video consultations and Space Finder have helped demonstrate the value of technology and data to help deliver a step-change in productivity, matching scarce clinical resource to a growing pool of demand.
There is now a huge opportunity (and need) to operationalise these techniques across local systems, pooling capacity to meet demand. This is challenging in data terms because of the need to consolidate disparate data sources across organisations to pinpoint where to focus, but advances in technology bring these opportunities within reach when systems are bold enough to drive the change.
