The business case for investing in health

 Tim Elwell-Sutton, Assistant Director of Strategic Partnerships at the Health Foundation, offers his insight on the impact of the social determinants of health, the cost of health inequalities and why, most crucially, it makes sense to invest in boosting health outcomes.
Tim Elwell-Sutton, Assistant Director of Strategic Partnerships at the Health Foundation, offers his insight on the impact of the social determinants of health, the cost of health inequalities and why, most crucially, it makes sense to invest in boosting health outcomes.
I got a letter recently from a new pension scheme I joined. It told me that I could start drawing my pension in 2044 – the year when I will turn 65. This raised two questions in my mind. First, what are the chances that I will be able to retire at age 65? (Answer: not good!) Second, what are the chances that I will be well enough to continue working beyond 65? Here, the odds are much better.
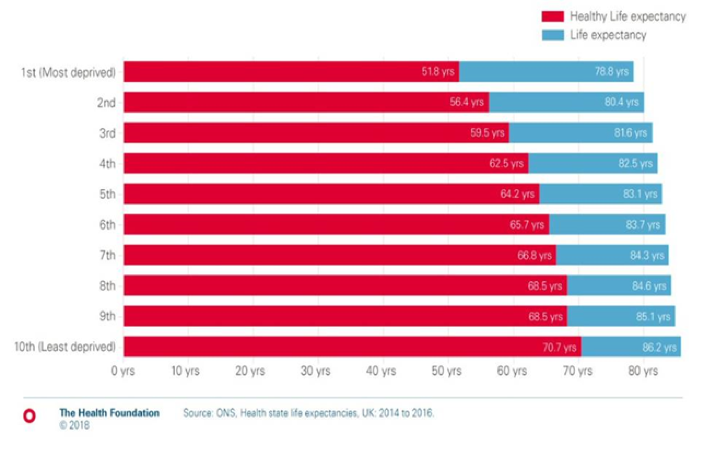
For someone of my socioeconomic profile, healthy life expectancy is well over 65. However, as Figure 1 shows, if you live in one of the most deprived parts of the country, the answer to that second question is quite different: healthy life expectancy for women in that group is just 51.8 (Figure1). That means they can expect, on average, to have 27 years of poor health at the end of life.
Is there a cogent business case for investing in health?
At a societal level, the case seems overwhelming if we invest in keeping people healthy, not just fixing them when they are already sick. This is vital because we know that the biggest influences on our health are not health services but the conditions in which we live, grow, work and age: the social determinants of health (Marmot 2010).
Investing in health does not just mean investing in the healthcare system. It means creating living conditions in which people can thrive physically, mentally and socially.
By contrast, public policy that is short-sighted and fails to take account of the wider determinants of health, has the potential to erode our quality of life and damage our productive potential. There are already worrying signs that the constant health improvements we have come to expect can no longer be taken for granted.
Life expectancy rises have stalled in recent years and life expectancy has actually started to decline in Scotland, Wales and Northern Ireland(see Figure 2), although these figures do not take account of possible health improvements in future cohorts. More worrying still, healthy life expectancy has failed to keep pace with life expectancy, particularly in more deprived areas.
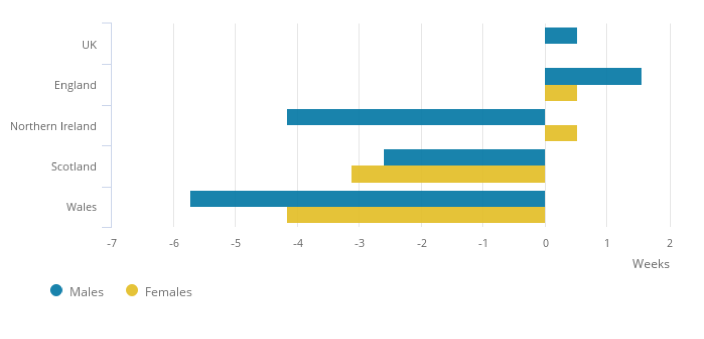
So, what kinds of investments keep people healthy and reduce costs to society? These range from traditional public health programmes such as tobacco control to complex interventions such as Sure Start children’s centres which support children and families at a crucial point in their lives.
However, in spite of evidence that these schemes have a positive impact, cuts to local authority budgets over the past 5 years have meant that investment in these services has declined substantially in recent years with spending on local tobacco control falling by 45 per cent between 2014-15 and 2018-19 (Finch 2018), and Sure Start spending falling by 59 per cent between 2009-10 and 2016-17 (Kelly 2018).
While there are clear social and economic incentives to keep people healthy, making the business case for specific interventions can be challenging. The causal pathways involved in population-level health interventions are often complex, making it more difficult to demonstrate clear links between intervention and outcome, or investment and return.
While this is difficult, it is not impossible. The Health Foundation is currently working with academic partners to develop and disseminate new methods for designing and evaluating the impact of interventions in complex systems.
Looking beyond individual services and interventions, there is also an important case to be made for investing in population health as an important contributor to economic and social outcomes.
Good health, in and of itself, enables people to have better enjoyment of their lives, of the goods and services they consume, and of the activities they undertake. Health can be a key determinant of the social and economic outcomes of individuals and of the places in which they live. Ongoing research funded by the Health Foundation is estimating the impact health has on such outcomes to better inform policy.
The case for investing in healthcare has been made very effectively in recent years with spending on the NHS set to rise from 20 per cent of total government spending in 2000 to 38 per cent by 2023-2024 (Zaranko 2018). Making the case for investing in keeping people healthy is, in many ways, more challenging but the prize – a healthier, more productive society which allows people to flourish – is one worth fighting for.
References
Abelson, P., R. Taylor, J. Butler and Ageing (2003). Returns on investment in public health. Canberra, Department of Health and Aging.
Finch, D. B., Joanne; Elwell-Sutton, Tim (2018). Briefing: Taking our health for granted. London, The Health Foundation.
Gaheer, S. P., Gillian (2016). The value for money of children’s centre services: Evaluation of children’s centres in England (ECCE) Strand 5. D. f. Education, Department for Education; Frontier Economics.
Godfrey, C., S. Parrott, T. Coleman and E. Pound (2005). “The cost-effectiveness of the English smoking treatment services: evidence from practice.” Addiction 100(s2): 70-83.
Kelly, E. L., Tom; Sibieta, Luke; Waters, Tom (2018). Public Spending on Children in England: 2000 to 2020, Institute for Fiscal Stuides;
Children’s Commissioner.
Marmot, M. (2010). Fair society, health lives: Strategic review of health inequalities in England post 2010. London.
Office for National Statistics (2018). National life tables, UK: 2015 to 2017. Statistical Bulletin. London, ONS.
Richard, P., K. West and L. Ku (2012). “The return on investment of a Medicaid tobacco cessation program in Massachusetts.” PLoS One7(1): e29665.
Rutter, H., N. Savona, K. Glonti, J. Bibby, S. Cummins, D. T. Finegood, F. Greaves, L. Harper, P. Hawe, L. Moore, M. Petticrew, E. Rehfuess, A. Shiell, J. Thomas and M. White (2017). “The need for a complex systems model of evidence for public health.” The Lancet 390(10112): 2602-2604.
Zaranko, B. (2018). The end of austerity? Institute for Fiscal Studies, IFS.
